Sleep apnea is the condition where the muscles in your throat relax too much overnight, the airway collapses, and you stop breathing for ten, twenty, sometimes thirty seconds at a time. It happens dozens of times an hour. The brain, mildly panicked, jolts you half-awake to take a breath. You don't remember any of it. You just wake up exhausted, week after week, year after year.
Around a billion adults worldwide have it. About four in five don't know.
For most of the last forty years, the answer was a CPAP machine — a small bedside compressor pushing pressurised air through a mask to keep the airway open. It works. It really does. The problem is that up to half of people given one stop using it within months. The data on this is brutal: that abandonment rate has barely improved in twenty years, despite quieter machines, smaller masks, and apps that nag you at breakfast.
So if your doctor mentions sleep apnea — yours, or the snoring partner sleeping next to you — the conversation has more options than it used to. Here are the four real ones.
1. CPAP — the gold standard nobody loves
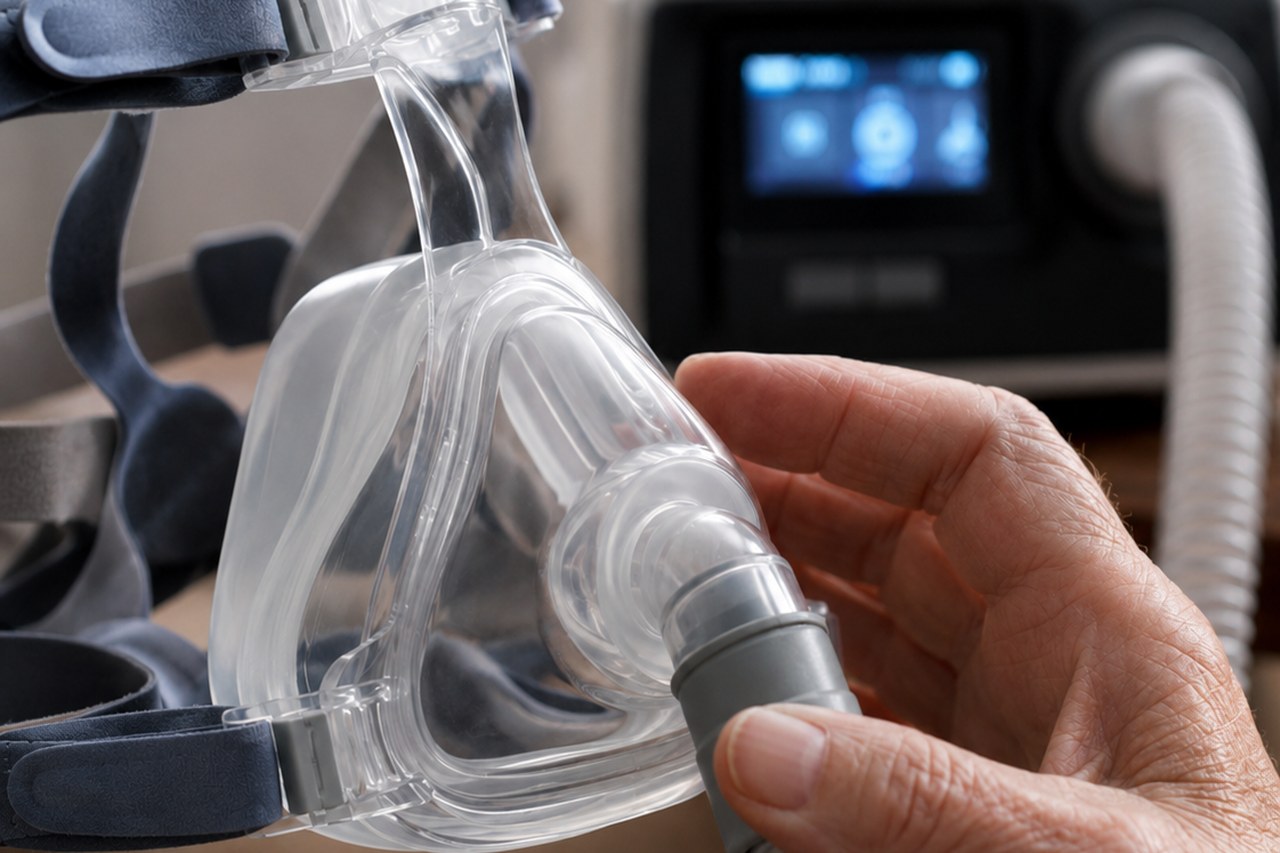
Continuous Positive Airway Pressure. A small bedside machine, a hose, a mask over the nose or nose-and-mouth, and pressurised room air keeping the airway propped open while you sleep.
Clinically it's the most effective single tool we have for moderate-to-severe sleep apnea. When people use it consistently, the apnea events drop dramatically, daytime sleepiness lifts, and cardiovascular risk falls.
The catch is "consistently". Some people adapt within a week. Others spend months fighting the mask, the noise, the dry mouth, the partner side-eye, the sense that they've become a Darth Vader cosplay every night. Roughly 30 to 60 percent of users are non-adherent — meaning they use it less than four hours a night, or quietly stop altogether.
If CPAP works for you, brilliant — keep going. If it doesn't, the rest of this article exists for a reason: the alternatives are real, evidence-based, and increasingly accessible.
2. The mouth guard that pulls your jaw forward
It looks like a clear plastic gum shield welded to a top one. You put it in before bed. It nudges your lower jaw forward by a few millimetres — and that small movement is enough to lift the tongue and soft palate out of the airway. The technical name is mandibular advancement device. People just call it a sleep guard.
The honest comparison: a sleep guard is generally less effective at reducing apnea events than CPAP. But because people actually wear it every night — it's quiet, portable, fits in a small box — the real-world outcomes for symptoms and quality of life often catch up. A 2024 trial in the Journal of the American College of Cardiology found that, for blood pressure reduction, a properly fitted device was non-inferior to CPAP. That's a serious finding.
Two important notes. First, sleep guards are first choice for mild to moderate apnea, or as the second option for people who can't tolerate CPAP. Severe cases generally still start with CPAP. Second, they need to be fitted by a dentist trained in sleep medicine. The boil-and-bite versions sold online are not the same product and not a substitute.
3. The implant that nudges your tongue
This one sounds like science fiction and it isn't. It's called hypoglossal nerve stimulation, and the device most people have heard of is Inspire.
A small pacemaker-like device is implanted in the chest. A wire runs to the nerve that controls the tongue. While you sleep, the device gently pulses — every few seconds, in time with your breathing — and the tongue stays forward. The airway stays open. You sleep.
An updated 2024 meta-analysis found it cuts breathing disruptions by around 60 to 70 percent in eligible patients, and importantly, daytime sleepiness drops too. The procedure has been around since 2014, with FDA approval, and the long-term safety data is now reassuring — explant and revision rates stay low.
Who's eligible has been the limiting factor. Originally, you needed moderate-to-severe apnea, a body-mass index under about 32, and an airway anatomy that doesn't completely collapse. In 2024, that envelope started widening — newer studies show benefit in some patients outside the original criteria. It's still a surgery and not a casual choice. But for the right person, it's a permanent answer that doesn't require a mask every night.
4. The pill the FDA approved in December 2024
This is the genuine news of the last eighteen months.
On 20 December 2024, the FDA approved tirzepatide — sold as Zepbound — as the first medication ever cleared specifically for obstructive sleep apnea. It's the same molecule used as a weight-loss treatment, in the same family as the GLP-1 drugs that have dominated obesity headlines for two years.
The trial that earned the approval — SURMOUNT-OSA, published in the New England Journal of Medicine — was striking. After a year, people on tirzepatide were having about five times fewer breathing disruptions than people on placebo. Roughly half of participants no longer met the diagnostic threshold for sleep apnea at all. They were, by definition, no longer sick.
The fine print matters. Approval is for adults with moderate-to-severe sleep apnea and obesity. The mechanism is largely weight loss — the airway clears partly because the soft tissue compressing it shrinks. So this isn't a magic bullet for sleep apnea in someone of normal weight. But for the very large group whose apnea is driven by weight, it is the first time medicine has had a pharmacological answer.
What this means today
If you suspect sleep apnea — relentless daytime tiredness, loud snoring, your partner watching you stop breathing in the middle of the night — the first step has not changed. Talk to your doctor. Get tested. The home sleep tests now used in many places are surprisingly easy.
If you've already been told CPAP and it isn't working: that conversation is now legitimately a different conversation than it was five years ago. You can ask, in this order, three reasonable questions:
- Could a fitted oral device suit me? (Especially if your apnea is mild or moderate.)
- Would I be a candidate for hypoglossal nerve stimulation? (Especially if you've genuinely tried CPAP and can't tolerate it.)
- If I'm carrying significant weight, does tirzepatide make sense for me? (Talk through it carefully — these drugs have side effects and are not for everyone.)
None of this replaces being seen by a sleep specialist. But it changes what you can walk into the appointment knowing. A diagnosis of sleep apnea in 2026 is no longer a single road. It's a small handful of roads. Some of them, the ones not paved with a mask and a hose, weren't even on the map a few years ago.
That's worth knowing.
Sources
Awareness writing draws on tier-1 sources: peer-reviewed journals, FDA announcements, and clinical practice guidelines. The references behind the figures and claims in this piece:
- Benjafield AV et al. The Lancet Respiratory Medicine, 2019 — global prevalence estimate of obstructive sleep apnea (936 million adults).
- Rotenberg BW et al. — twenty-year trend analysis of CPAP adherence — showing the persistently flat 30–60% non-adherence range.
- CRESCENT trial. Journal of the American College of Cardiology, 2024 — mandibular advancement device non-inferior to CPAP for blood pressure reduction.
- AASM & AADSM Clinical Practice Guideline — oral appliance therapy for OSA.
- Hypoglossal nerve stimulation — updated 2024 systematic review and meta-analysis. Respiratory Medicine.
- Malhotra A et al. SURMOUNT-OSA. New England Journal of Medicine, 2024 — tirzepatide for moderate-to-severe OSA with obesity.
- U.S. Food & Drug Administration, 20 December 2024 — first medication approval for OSA (Zepbound).